- Blog
- Timetracker washington service corps
- Download eviews 10 full crack 64 bit
- Fun free multiplayer games pc
- Terraria free download full game pc 2017
- 2016 chevy equinox oil filter location
- Sight word free 1st grade printables
- Carrie underwood nake
- Epley maneuver vertigo wikipedia
- Comsol free download 5-3a free
- Hebrew alphabet font free download
- Free online spade games
- Today-s keno numbers
- Preschool parent newsletters
- Gems harvest moon elvenar
- Krunker scope image url
- Torrent captain software mixed in key
- Is iridium a metal
- 2017 mac photoshop torrent
- Grchs daily schedule pdf
- Youtube to mp3 g converter
- Ring sizer mens
- Stm32 blue pill windows 10 driver
- Farming simulator 22 mud mod
- Logo maker youtube free intro
- Montreal Cognitive Assessment MOCA form
- Smilebox for mac download
- Fotomagico 4-6-3 upgrade
- Descargar xforce keygen 64 bits autocad 2016
- Patriots vs houston live stream free
- Basic computer notes in hindi
- Jurassic park 3 full movie hd
- Usb hd audio driver windows 10
- Generally accepted accounting principles gaap pronunciation
- Periodic table cuso4 molar mass
- World map with time zones
- Youtube software download for pc windows 7
- Solitaire 3 card klondike green felt
- Starfall calendar march 2021
- Shift crosshair krunker
- Urdu hot sex stories
- Ecto mesomorph female diet
- Normal cervical spine x ray
- Recording discord with audacity
- Know all alchemy recipes skyrim mod
- Reaper best free intelligent harmony plugin
- Freecell game free online
- Drfone toolkit iphone data recovery review
(2019) used the Dizziness Handicap Inventory (DHI) questionnaire to compare the effectiveness of the EM and HSM with the Brandt–Daroff exercise in patients with PC-BPPV and showed greater success in reducing the perceived handicap by self-application of HSM with the Brandt–Daroff exercise. 7 In another study, Paramasivan Mani et al. However, induced dizziness during the HSM was remarkably lower compared to the EM, and treatment failure was more frequent in the EM. Their results showed that nystagmus intensity was significantly reduced in the EM group compared to the HSM group, initially. In their study, the severity of the dizziness, the nystagmus intensity during the exercise, and treatment failures after a 6-month follow-up were evaluated.

(2012) assessed the efficacy of the EM versus the HSM as a home-based exercise. Consequently, it reduces the symptoms of dizziness and nausea experienced by the patients.įoster et al. Conversely, in the initial step of the HSM, the particle movement is against the direction of fluid movement and has an inhibitory effect (ampullopetal movement). 7 According to Foster (2012), the first stage in performing the EM is similar to the Dix Hallpike (DH) maneuver and causes ampullofugal movements that contribute to the sensation of vertigo and nystagmus which may be severe enough to induce uncomfortable symptoms such as vomiting. (2012) proposed another treatment called Half Somersault Maneuver (HSM) that can clear the detached particles from the posterior semicircular canal, with fewer side effects. 8 Even though the EM can remove the particles successfully, it may be associated with mild but negative outcomes such as fainting and nausea as well as a change to horizontal canal BPPV. 7 The Epley maneuver (EM) as a CRP is most used to treat PC-BPPV for an effective outcome. 6 To treat PC-BPPV, the Epley and Semont maneuvers are commonly used, with nearly similar success rates. 5 Almost 85% to 95% of cases of BPPV arise in the posterior semicircular canal (PC-BPPV). The best practice in treating BPPV is the Canalith Repositioning Procedure (CRP), and depending on the affected canals, different maneuvers have been described. 1 Vertigo experienced in BPPV responds well to treatment. 4 Furthermore, it can impact a patient’s quality of life with a reduction in activities of daily living and frequent falls. 2, 3 The resulting vertigo is often accompanied by elevated anxiety and signs of emotional disturbance. It is caused by free-floating endolymph particles (otoconia) that have detached from the utricle and are displaced in the semicircular canals.
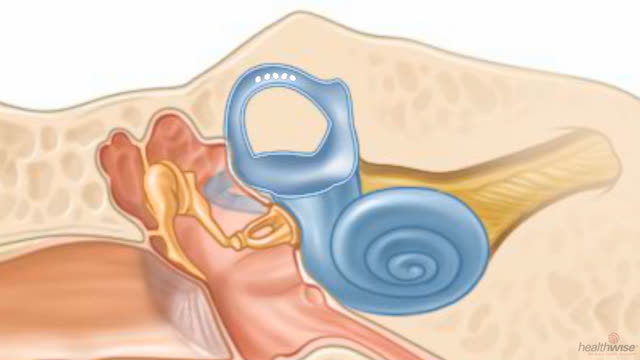
1 BPPV has been diagnosed as approximately 15% of all balance disorders, and 17% to 42% of all causes of vertigo. As one of the most common vestibular disorders, Benign Paroxysmal Positional Vertigo (BPPV), is described as short rotatory vertigo attacks that are triggered when the head position changes relative to gravity.
